Tampa Nursing Home Abuse & Neglect Lawyers | Legal Guide
Florida Elder Justice and Facility Litigation: A Comprehensive Analysis of Tampa-Based Representation, Statutory Frameworks, and Pressure Ulcer Settlements

The institutionalization of elder care in the United States has necessitated rigorous, highly scrutinized regulatory frameworks designed to protect an exceptionally vulnerable demographic. In the state of Florida, particularly within the rapidly expanding metropolitan hub of Tampa and the broader Hillsborough County region, the intersection of a surging aging population and a heavily corporatized healthcare sector has precipitated complex legal battlegrounds. Demographic data establishes that Tampa is a rapidly growing municipality of approximately 377,000 residents situated on Florida’s Gulf Coast, encompassing historic neighborhoods such as Ybor City and sprawling suburban tracts. Crucially, 23% of Tampa households currently house a resident over the age of 55, with more than 17,000 residents aged 65 and older. Like many major Florida municipalities, this concentration of elderly citizens has catalyzed the proliferation of skilled nursing facilities (SNFs) and assisted living facilities (ALFs).
Consequently, the Tampa Bay region has witnessed a corresponding escalation in allegations of institutional neglect, medical malpractice, and systemic abuse, driven by systemic understaffing and corporate cost-cutting measures. Securing a specialized nursing home abuse lawyer Tampa residents can trust has become an imperative for families navigating the devastating aftermath of preventable injuries, ranging from advanced pressure ulcers (bedsores) and malnutrition to catastrophic falls and wrongful death. This exhaustive research report provides a granular examination of the statutory mechanisms governing Florida elder care facilities, the procedural mandates for initiating litigation, the clinical and evidentiary pathology of pressure ulcer claims, the current valuation of lawsuit settlements, recent legislative transformations in 2025 and 2026, and the strategic methodologies employed by preeminent elder neglect attorneys operating within the Tampa Bay jurisdiction.
The Demographic and Corporate Landscape of Tampa Elder Care
The fundamental root cause of the vast majority of facility neglect within Florida is systemic understaffing and inadequate clinical training. The elder care industry is heavily saturated with for-profit corporations and private equity firms that frequently prioritize “cash over care,” operating under purposefully complex and multilayered corporate regimes designed specifically to subvert the justice system and shield assets. To maximize profit margins, corporate management intentionally operates facilities with a minimal crew of lower-paid, under-qualified nursing assistants. When a facility is critically understaffed, a well-meaning nurse or aide may be forced to allocate as little as 10 minutes of direct, hands-on care to each highly compromised resident during a given shift.
This corporate architecture directly yields catastrophic clinical outcomes within Hillsborough County. The region contains a dense network of facilities where such incidents frequently occur. The following table identifies several prominent nursing homes and ALFs operating within the greater Tampa area that are subject to the statutory frameworks discussed herein:
| Facility Name | Location | Facility Type/Focus |
|---|---|---|
| Allegro | 16001 Lakeshore Villa Dr, Tampa, FL 33613 | Assisted Living / Senior Living |
| Angels Senior Living at South Tampa | 3330 S MacDill Ave, Tampa, FL 33629 | Assisted Living Facility |
| Bayshore Pointe Nursing and Rehab Center | 3117 W Gandy Blvd, Tampa, FL 33611 | Skilled Nursing / Rehabilitation |
| The Bristol at Tampa Rehabilitation & Nursing Center | 1818 E Fletcher Ave, Tampa, FL 33612 | Skilled Nursing / Rehabilitation |
| Cameron ALF III | 3202 W Minnehaha St, Tampa, FL 33614 | Assisted Living Facility |
| Central Tampa Assisted Living | 5010 N 40th St #5202, Tampa, FL 33610 | Assisted Living Facility |
| Community Care Center | 2202 W Oak Ave, Plant City, FL 33563 | Skilled Nursing / Long-Term Care |

Within these facilities, the manifestations of corporate neglect are ubiquitous. Residents who cannot feed themselves are routinely left with untouched food trays, leading to rapid dehydration and fatal malnutrition. When staff members are unavailable to assist residents with toileting or transferring from a bed to a wheelchair, residents predictably attempt these movements independently, resulting in falls that cause hip fractures, traumatic brain injuries, or fatal subdural hematomas. Furthermore, understaffed nurses facing impossible administrative burdens inevitably commit medication errors, either by administering the incorrect dosage, giving medication to the wrong patient, or entirely missing vital therapeutic windows. In facilities housing dementia patients, failures in supervision and environmental security frequently lead to wandering and elopement, exposing cognitively impaired residents to fatal environmental hazards.
Statutory Governance: Chapter 400 and Skilled Nursing Facilities
The foundation of any skilled nursing facility negligence claim in Florida is rooted in Chapter 400 of the Florida Statutes. This chapter imposes strict mandates on operational conduct, patient care, and administrative accountability. A cornerstone of this legislative framework is the Florida Nursing Home Residents’ Rights Act, codified under § 400.022. This statute operates not merely as a set of suggested best practices, but as a binding legal requirement that every facility—whether funded by Medicare, Medicaid, or private payment—must strictly adhere to under penalty of law.
The Residents’ Rights Act guarantees fundamental protections that directly target the abuses frequently observed in institutional settings:
- Emotional and Psychological Protection: Residents have the explicit right to be treated with dignity and respect. Facility staff are legally prohibited from yelling at, threatening, or emotionally abusing residents, even when cognitive conditions such as advanced dementia render patient care exceedingly challenging.
- Chemical and Physical Restraint Protection: Facilities are categorically barred from utilizing psychotropic medications or physical restraints for the mere convenience of the staff or to make residents easier to manage. Chemical restraints must be strictly medically necessary, properly monitored by a prescribing physician, and routinely evaluated for efficacy and necessity.
- Financial Protection and Fiduciary Duty: Staff and administration cannot lawfully take or commingle a resident’s money, personal belongings, or Social Security benefits. Nursing homes must establish and maintain an accounting system that explicitly prevents the commingling of a resident’s personal funds with facility capital or the funds of other residents. This accounting must be conducted according to generally accepted accounting principles (GAAP), and a quarterly accounting of any transaction made on behalf of the resident must be furnished to the resident or their legal representative.
Violations of Chapter 400 trigger multifaceted consequences. State agencies, such as the Florida Agency for Health Care Administration (AHCA), maintain the authority to investigate complaints and levy administrative fines up to $10,000 per violation. They possess the ultimate authority to shut down nursing homes that demonstrate a pattern of repeated rights violations. Furthermore, the State Long-Term Care Ombudsman Program plays a vital oversight role. Under the statutes, a representative of the Ombudsman Program is mandated to identify and investigate complaints made by or on behalf of a resident within a reasonable timeframe. The duties of the legal advocate within this program include pursuing administrative and legal remedies on behalf of residents, assisting the state ombudsman with respect to exploitation or abuse, and analyzing and commenting on the development of federal, state, and local laws pertaining to long-term care.
To protect those who expose these systemic failures, Florida law provides explicit immunity. Any person who submits a complaint concerning suspected rights violations, or who testifies in any administrative or judicial proceeding arising from such a complaint, is granted immunity from criminal or civil liability, provided they have not acted in bad faith or with malicious purpose. Despite these administrative safeguards, regulatory fines frequently fail to adequately compensate the victim or deter massive healthcare conglomerates. Thus, Chapter 400 grants residents and their families a private right of action to pursue civil lawsuits for compensatory and punitive damages resulting from rights violations or deviations from the applicable standard of care.
Chapter 429: The Assisted Living Facility (ALF) Paradigm
Assisted living facility litigation operates under a distinct, parallel statutory paradigm governed by Chapter 429 of the Florida Statutes, formally cited as the “Assisted Living Facilities Act”. While nursing homes provide 24-hour skilled medical care, ALFs are designed to offer a more homelike, least restrictive environment, providing housing, meals, and basic assistance with activities of daily living for individuals who do not require constant medical intervention.
Florida law explicitly establishes that an ALF inherently owes a lower duty of medical care compared to a skilled nursing facility. By statutory mandate, a standard ALF may not serve residents who require 24-hour nursing supervision. However, this lower duty of care is frequently manipulated by defense counsel during litigation.
The standard built-in defense whenever an adverse event occurs inside an ALF is the assertion: “We are an assisted living facility, not a nursing home”. Expert legal counsel counters this defense by highlighting the ALF’s rigid legal obligation to recommend discharge and transfer residents whose medical acuity levels have surpassed the facility’s capacity to provide safe care. If a resident suffers repeated falls, the facility cannot simply claim falls are unpreventable in an ALF; they must either implement appropriate interventions or discharge the resident to a higher care facility.
If an ALF intends to provide extended medical care, it must obtain specific specialty licenses from the AHCA. For example, a facility licensed to provide limited nursing services must maintain a written progress report on each person receiving such services, and the services must be medically complex enough to require constant supervision, assessment, or intervention by a licensed nurse on a daily basis. If an ALF has been licensed for less than two years, any initial extended congregate care license issued is strictly provisional and may not exceed six months.
Chapter 429 includes its own robust Resident Bill of Rights (§ 429.28). This statute ensures that no resident is deprived of civil or legal rights guaranteed by the State or Federal Constitution. Every resident possesses the right to live in a safe and decent environment, completely free from abuse and neglect. Furthermore, residents are guaranteed unrestricted private communication, including the right to receive unopened correspondence, access telephones, and visit with any person of their choice between the hours of 9 a.m. and 9 p.m. at a minimum, with provisions for extended hours for out-of-town guests and caregivers. When an ALF’s conduct demonstrates an intentional or reckless disregard for these rights or the resident’s safety—often driven by a corporate desire to retain the resident’s private, out-of-pocket payments rather than discharging them—plaintiffs’ attorneys may seek punitive damages against the facility under Florida Statute § 429.298.
The Procedural Labyrinth: Pre-Suit Notice and Statutes of Limitations
Litigating an elder abuse claim in Florida is a procedurally rigorous endeavor governed by strict timelines and notification mandates. Florida Statute § 400.0236 dictates a two-year statute of limitations for nursing home negligence cases. This means a plaintiff generally has exactly two years from the date the injury was discovered, or should have been discovered with the exercise of due diligence, to formally initiate a legal claim. The law also includes a statute of repose, dictating that under no circumstances can the statute of limitations be extended beyond four years from the date of the incident giving rise to the injury.
Crucially, an elder neglect attorney in Florida cannot immediately file a lawsuit in state circuit court upon retaining a client. Florida law mandates a complex, time-consuming pre-suit investigation and notification process under § 400.0233. Prior to filing a complaint for a violation of a resident’s rights or for negligence, the claimant must notify each prospective defendant via certified mail, return receipt requested. This pre-suit notification must explicitly identify the specific rights under § 400.022 that the prospective defendant violated, or describe the exact deviation from the standard of care, along with a brief description of the reasonably identifiable injuries sustained by the resident.
The issuance of this formal pre-suit notice triggers a mandatory 75-day waiting period, during which the statute of limitations is legally tolled for all prospective defendants. This 75-day window functions as a vital informal discovery period. Both the plaintiff and the defense are permitted to request unsworn statements from relevant parties and demand the production of relevant documents. By law, any responsive documents requested during this period must be produced within 20 days. If the nursing home, its corporate ownership, or its liability insurer fails to respond or offer a settlement within the 75-day period, the statute deems the claim rejected, thereby clearing the way for the plaintiff to formally file the lawsuit in court. Florida courts strictly enforce this pre-suit requirement; it is viewed as an absolute condition precedent to litigation, and any lawsuit filed without completely fulfilling the 75-day notice period is subject to immediate dismissal. Because gathering massive volumes of medical records, securing expert medical reviews, and determining complex corporate facility ownership can take months, attorneys strongly advise families to initiate legal contact well before the two-year deadline approaches.
Transformative 2025 and 2026 Legislative Developments in Florida Healthcare
The legislative landscape governing healthcare litigation in Florida is highly dynamic, with the recently adjourned 2025 and extended 2026 legislative sessions introducing profound changes to the state’s statutes. During these sessions, the Florida Senate and House leaders extended the session through June 6, 2026, primarily to pass the state budget, but this extension allowed for critical procedural maneuvers that revived vital policy bills affecting medical negligence and facility operations.
The most impactful development for personal injury and elder abuse practitioners was the passage of HB 6017, titled “Recovery of Damages for Medical Negligence Resulting in Death,” championed by Rep. Trabulsy and Sen. Yarborough. Prior to the passage of this bill, Florida maintained a highly controversial law—colloquially known as the “free kill” law—which strictly prohibited the adult children (over age 25) and the parents of adult victims from recovering non-economic damages (such as pain and suffering) in wrongful death medical malpractice claims. This draconian statute meant that if an elderly, unmarried resident without minor children was killed by egregious medical malpractice inside a facility, their surviving adult children had virtually no legal mechanism to recover meaningful non-economic damages. During the closing days of the extended session, HB 6017 was revived by a procedural maneuver and passed, fundamentally removing this prohibition in cases where the defendant is a hospital or healthcare practitioner. Because nursing home litigation frequently intersects with medical malpractice—especially when the negligence involves attending facility physicians or advanced practice registered nurses—this legislative repeal drastically expands the settlement and verdict potential for wrongful death claims.
Additional sweeping legislative changes included:
- SB 1404 (Memory Care Specialty License): This legislation mandates that any ALF serving memory care residents, or holding itself out to the public as providing memory care services, must obtain a new, specific memory care services specialty license. This establishes tighter regulatory oversight and specific clinical benchmarks over facilities housing dementia and Alzheimer’s patients, providing plaintiffs’ attorneys with clear statutory guidelines to cite during litigation when a cognitively impaired resident elopes or is injured.
- HB 1421 (Emily Adkins Family Protection Act): With an effective date of July 1, 2025, this bill radically improves screening and treatment measures for venous thromboembolism (VTE) and blood clots in Florida. It adds chronic obstructive pulmonary disease, chronic critical illness, and genetic predisposition to the list of chronic diseases under the state’s Chronic Diseases Act. Crucially for healthcare facilities, it requires the Department of Health to contract with a private entity to create a statewide VTE registry. Starting July 1, 2026, hospitals and ambulatory surgical centers must report specified information to the registry and implement rigorous training and protocols to assess patients at risk for deep vein thromboses.
- HB 1427 (Nursing Education Programs): Sponsored by Rep. Griffits, this bill was enacted to address Florida’s systemic issues with nursing education and the state’s alarmingly low passage rate on the national nursing examination (NCLEX). The bill dramatically strengthens the Board of Nursing’s oversight of educational programs by enhancing application requirements and imposing stricter accountability measures, ensuring that the pipeline of nurses entering ALFs and SNFs is adequately prepared.
- Failed Legislation: It is equally important to note bills that failed to pass, which shape the ongoing legal discourse.
HB 1083 (Patient Access to Records), which sought to create uniform guidelines for patient access to health records, died when time ran out in the Senate. Similarly, the proposed “Medical Freedom Act” and “Rural Renaissance” bills did not advance through the regular session.
Pathophysiology and Legal Valuation of Pressure Ulcers (Bedsores)
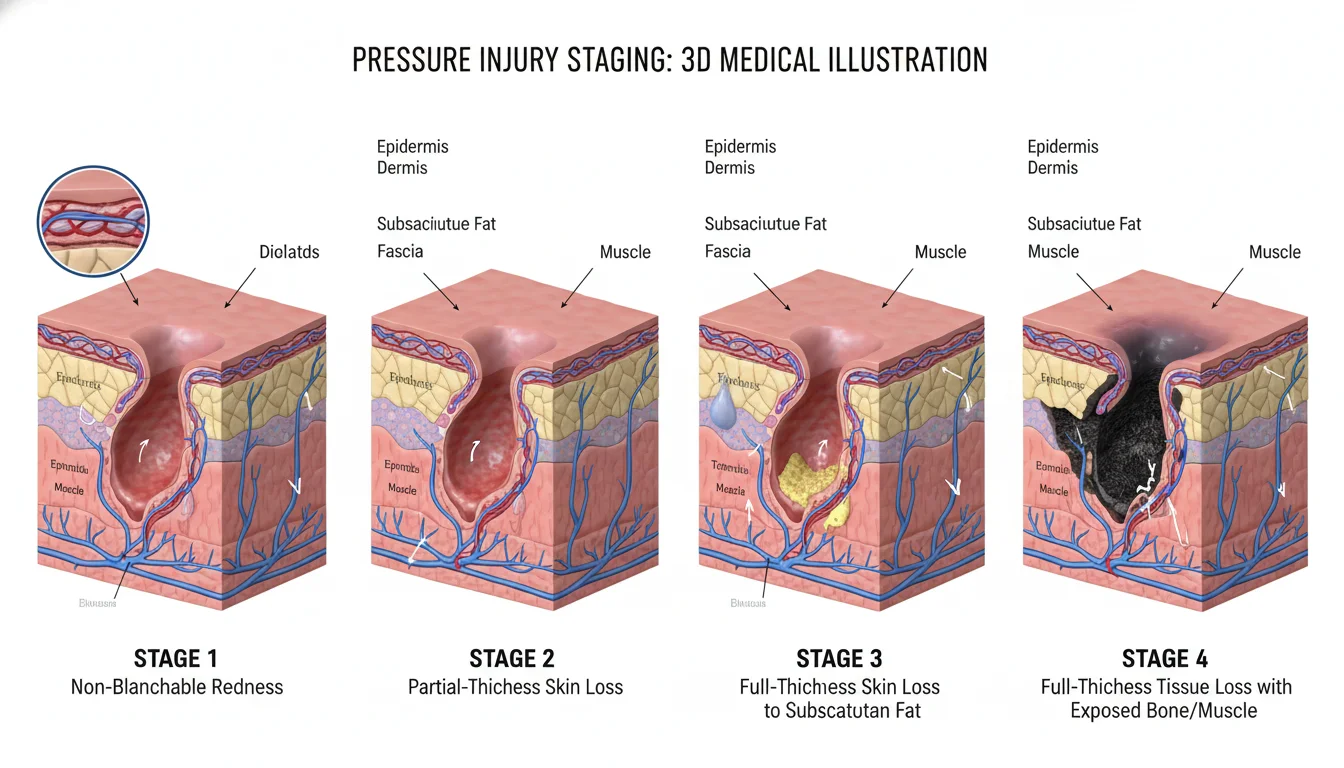
Perhaps the most definitive, medically undeniable indicator of profound institutional neglect is the development of a severe pressure ulcer, commonly referred to as a bedsore or decubitus ulcer. These ischemic injuries occur when prolonged, unrelieved pressure—typically focused over bony prominences such as the sacrum, coccyx, heels, or shoulder blades—compresses the capillary beds, effectively cutting off arterial blood flow to the skin and underlying subcutaneous tissues. Deprived of oxygen and vital nutrients, the tissue undergoes rapid cellular death and necrosis.
The Clinical Staging of Pressure Injuries
The clinical staging of a bedsore is the single most influential variable in determining the trajectory, defense strategy, and ultimate financial value of a Florida bedsore claim. The medical and legal communities, adhering to the National Pressure Injury Advisory Panel (NPIAP) guidelines, classify these wounds into four primary stages of escalating severity:
- Stage 1: The affected area of skin remains completely intact but appears visibly red (erythema) and feels warm to the touch. Crucially, the redness does not blanch (turn white) when physical pressure is temporarily applied, indicating early-stage tissue damage.
- Stage 2: The outer layer of the skin (epidermis) and part of the underlying dermal layer wear away, forming an open, shallow wound or a fluid-filled blister.
- Stage 3: The ulcer progresses into a deep crater, representing full-thickness skin loss. Subcutaneous fat is frequently visible within the wound bed, though bone, tendon, or muscle is not yet exposed. Slough (dead tissue) or eschar (a dark scab) may be present.
- Stage 4: The wound involves catastrophic, full-thickness tissue loss with exposed, palpable bone, muscle, tendon, or cartilage. These profound wounds frequently become highly necrotic and carry a massive clinical risk of osteomyelitis (deep bone infection) and fatal systemic sepsis. Patients suffering from Stage 4 ulcers inevitably require brutal surgical debridement, advanced wound vacs, and prolonged rehabilitation to restore any semblance of their original quality of life, assuming recovery is even physiologically possible.
Evidentiary Methodologies in Proving Corporate Neglect
In the realm of medical malpractice and elder law, severe bedsores are overwhelmingly viewed as preventable. The universally accepted standard of care mandates that immobile residents must be repositioned by clinical staff at a minimum of every two hours, placed on specialized pressure-relieving air mattresses, continuously monitored for skin integrity, and kept scrupulously clean from the highly caustic effects of urinary and fecal incontinence. Consequently, advanced Stage 3 and Stage 4 bedsores are recognized in the healthcare sector as “never events”—a class of medical error that should simply never occur if basic, proper clinical protocols are followed.
Defense attorneys representing nursing homes invariably attempt to construct a medical defense arguing that the ulcer was clinically unavoidable. They routinely blame the resident’s advanced age, pre-existing co-morbidities (such as diabetes or peripheral artery disease), and ostensibly poor natural nutrition. To systematically dismantle this defense, an expert nursing home abuse lawyer in Tampa will immediately subpoena the facility’s repositioning logs and flowsheets. Missing, fabricated, or incomplete turn logs make it exceedingly difficult for the defense to argue before a jury that no neglect occurred. Furthermore, top-tier plaintiffs’ attorneys counter the “poor nutrition” defense by obtaining the patient’s albumin and pre-albumin laboratory data; if the lab results irrefutably prove that the patient’s protein levels were adequate prior to the wound’s development, the defense’s entire argument collapses.
When a Stage 4 bedsore develops, it provides the plaintiff with irrefutable, physical evidence of prolonged, systemic neglect, as a wound of that depth takes days or weeks of continuous, unbroken inattention to form. In these egregious scenarios, plaintiffs’ counsel will aggressively secure the facility’s internal corporate payroll records. By correlating the facility’s daily staffing levels against patient census data on the exact dates the bedsore developed, attorneys can mathematically prove that the facility was operating with chronic understaffing. This evidentiary presentation of corporate cost-cutting at the expense of human life exposes the facility to massive punitive damages under Florida Statute § 400.0237, fundamentally shifting the financial exposure of the defendant.
Academic analyses, such as those evaluating malpractice claims associated with pressure ulcers, underscore the correlation between facility administration and patient outcomes. Studies evaluating for-profit Medicare home health and nursing agencies repeatedly demonstrate that corporate models prioritizing higher profit margins inherently deliver lower quality care, directly culminating in increased incidence of ischemic injuries and wrongful death. Data from 2019 legal database studies reveals that among bedsore lawsuits, an overwhelming 75.9% of cases were directly related to negligence, while 22.7% were classified strictly as medical malpractice. The most common defendants in these actions are hospitals (61.7%), nursing homes (31.2%), and individual medical providers (7.1%).
Landmark Case Studies and Settlement Averages
Determining an exact “average” bedsore lawsuit settlement amount is inherently complex, as every individual case features distinct medical expenses, varying degrees of conscious pain and suffering, and shifting jurisdictional dynamics. However, national databases and Florida-specific litigation records provide clear valuation ranges, primarily predicated on the clinical stage of the wound and the degree of provable corporate malfeasance.
Nationwide, some legal databases calculate the average bedsore settlement in nursing home lawsuits at approximately $1,616,228, though a more conservative baseline average for cases resulting in severe harm is generally cited near $400,000. When cases proceed to trial, verdicts are in favor of plaintiffs in 34.8% of cases, while the defense prevails in 36.2% of cases, highlighting the inherent risks of litigation and the necessity of highly skilled counsel. Approximately 25.5% of all bedsore lawsuits resolve via private settlement prior to a jury verdict.
The following table synthesizes typical Florida settlement ranges, correlating the clinical stage of the injury with standard defense weaknesses and financial payouts:
| Clinical Bedsore Stage | Typical Florida Settlement Range | Key Case Characteristics & Evidentiary Defense Weaknesses |
|---|---|---|
| Stage 1 to Stage 2 | $10,000 to $250,000 | Resident typically recovers without severe long-term harm. Liability is established via missing or incomplete repositioning logs, making it hard for the defense to argue “no neglect.” |
| Stage 3 | $100,000 to $750,000 | Deep crater wounds requiring painful debridement. Defenses blaming “poor nutrition due to age” are effectively disproved with albumin and pre-albumin lab data. |
| Stage 4 | $500,000 to $2,000,000+ | Catastrophic tissue loss exposing bone; often requires surgery or wound vacs. Classified as a clinical “never event,” making it highly indefensible. Juries rarely excuse wounds this deep. |
| Wrongful Death | $1,000,000 to $12,000,000+ | Sepsis or osteomyelitis originating from the ulcer acts as the primary or contributing cause of death. High punitive damage exposure under § 400.0237, often provable through facility payroll records demonstrating intentional understaffing. |
Florida juries have historically demonstrated a willingness to award staggering compensatory and punitive damages when faced with egregious, documented corporate neglect. A review of seminal Florida case studies and prominent national outcomes reveals the following landmark verdicts and settlements:
- $17,000,000 Verdict: Awarded in a Florida wrongful death claim involving a resident who suffered from deliberate starvation and an unmitigated Stage 4 bedsore.
- $14,000,000 Settlement: A massive settlement achieved after a Florida woman, placed in a nursing home following surgery, developed catastrophic pressure ulcers due to a complete lack of mobility assistance and basic hygiene.
- $12,800,000 Verdict: A wrongful death claim resulting from a facility’s total failure to treat bedsores or reposition an immobile patient on a regular schedule.
- $11,050,000 Verdict: A Miami-Dade Circuit Court jury awarded this sum to a plaintiff whose statutorily mandated resident rights were violated. Plaintiffs’ counsel presented touching testimony and facts-based analysis by a medical expert highlighting negligence that led to a severe brain injury.
- $7,810,000 Settlement: A highly complex case involving a 57-year-old woman who initially suffered severe injuries in a tractor-trailer accident, but later passed away due to profound neglect and the development of bedsores at a nursing facility during her recovery.
The settlement held both the trucking company and the healthcare facility financially accountable.
- $3,100,000 Verdict: Awarded in a case involving a wrongful death directly attributable to a pressure sore.
- $2,333,000 Verdict: Awarded for a preventable facility fall that resulted in a severe traumatic brain injury.
- $2,100,000 Settlement: Awarded to a 70-year-old resident who developed a Stage 4 bedsore in an Auburndale, Florida facility.
- $1,800,000 Settlement: Secured on behalf of a 61-year-old Florida resident who developed fatal sepsis originating from an untreated wound.
- $1,300,000 Verdict/Settlement: A prominent Florida outcome for the starvation of a 65-year-old nursing home resident. Another $1.3 million was awarded to the family of a resident who wandered away from a facility and died from environmental exposure.
For broader national context regarding the punitive exposure facing negligent facilities, a Philadelphia jury notably awarded $60 million in compensatory damages and a staggering $140 million in punitive damages in a landmark nursing home neglect verdict handled by the firm Munley, Munley & Cartwright, illustrating the extreme financial jeopardy corporations face when systemic abuse is proven before a jury.
Preeminent Legal Advocates in the Tampa Bay Jurisdiction
The profound complexities of Florida’s pre-suit notice requirements, the necessity for specialized medical expert testimony (including wound care specialists and medical directors), and the immense financial resources of corporate healthcare defense firms dictate that plaintiffs retain highly specialized, deeply resourced legal counsel. A premier elder neglect attorney in Florida must possess not only an encyclopedic understanding of Chapters 400 and 429 but also a proven, verifiable track record of securing multimillion-dollar verdicts that compel corporate accountability. The Tampa Bay region is serviced by a select echelon of such trial attorneys and boutique law firms, whose backgrounds, geographic footprints, and historic case outcomes are detailed below.
Ford, Dean & Rotundo, P.A.
Operating statewide with a predominant footprint in South Florida and the Tampa region, Ford, Dean & Rotundo is a niche law firm exclusively dedicated to nursing home abuse, assisted living facility neglect, and catastrophic medical malpractice. The firm’s local office is situated in North Miami Beach, but they heavily service the entire state, having protected elderly individuals in Florida since 1976.
Managing Partner William A. Dean is a formidable, nationally renowned presence in this sector. Admitted to the bar in 1997, Dean possesses a highly decorated background; he is an inducted member of the Union College Athletic Hall of Fame as the starting offensive guard on the 1989 Undefeated Football Team of Distinction, and he graduated cum laude from New York Law School, where he was inducted into the Order of the Bannisters. Dean began his legal career as an attorney at the Miami-Dade State Attorney’s Office, where he founded the Special Operations – Special Narcotics Unit, investigating violent felony crimes of organized drug traffickers. This profound background in investigating complex, organized, multi-layered criminal operations translates directly to his current practice of unravelling the corporate regimes of negligent nursing homes. Dean is Board Certified in Civil Trial Advocacy by the National Board of Trial Advocacy and has achieved the highest possible Martindale-Hubbell AV Preeminent peer-review rating. His firm has obtained over $100 million in verdicts and settlements for victims of abuse, including the $17 million wrongful death/Stage 4 bedsore verdict, the $11.05 million brain injury verdict against Coral Reef Operating LLC, and a $2.4 million settlement for an ALF neck fracture resulting from a series of falls.
Whittel & Melton, LLC
Maintaining a prominent satellite office in Tampa (located at 4401 W Kennedy Blvd #250) alongside multiple locations across Florida including Spring Hill, Gainesville, and Clearwater, Whittel & Melton operates as a heavyweight in the realm of personal injury, medical malpractice, and nursing home abuse. Partners Jason M. Melton and Robert G. Whittel boast impeccable peer ratings, including Avvo 10/10 ratings, continuous recognition by Super Lawyers, and membership in the prestigious Multi-Million Dollar Advocates Forum. Melton, a graduate of The Catholic University of America Columbus School of Law, is frequently cited in client reviews as an honest “straight shooter” who fights aggressively to ensure best-in-class representation.
Whittel & Melton’s litigation strategy involves a relentless deconstruction of the defense’s corporate structure. They publicly argue that modern nursing homes and ALFs utilize purposefully complex and multilayered corporate regimes designed explicitly to subvert the justice system and shield liquid assets. Their practice targets the underlying causes of neglect—specifically chronic understaffing and undertraining driven by a “cash over care” corporate philosophy. The firm is known for pursuing both compensatory and punitive damages for bedsores, overmedication, dehydration, and avoidable falls. The firm’s historic clinical negligence outcomes underscore their capacity for handling complex medical pathology, having secured:
- $1,650,000 for failure to diagnose and treat arterial clotting.
- $1,590,000 for food poisoning resulting in death.
- $1,500,000 for failure to diagnose bowel perforation following bariatric surgery.
- $1,475,000 verdict for lack of informed consent and negligence during an appendectomy.
- $1,150,000 for improper anesthesia administration during oral surgery.
- $1,070,000 for improper suturing of the renal artery in a kidney transplant.
- $575,000 explicitly for nursing home negligence involving pressure ulcers and death.
Gunn Law Group, P.A.
Situated in downtown Tampa at 401 East Jackson Street, the Gunn Law Group provides elite representation in catastrophic medical malpractice, personal injury, and nursing home neglect cases. The firm is led by Lee D. Gunn IV, a Board Certified Civil Trial Lawyer (certified by both The Florida Bar and the National Board of Trial Advocates) who possesses an AV Preeminent rating from Martindale-Hubbell and recurrent recognition by Super Lawyers and Best Lawyers in America.
Gunn’s professional background provides a distinct strategic advantage during complex litigation; prior to transitioning to plaintiff representation in 2000, he spent 17 years aggressively defending insurance companies, hospitals, product manufacturers, and major corporations. This extensive defense experience allows the firm to anticipate, deconstruct, and dismantle the tactics utilized by facility insurers. Gunn is also a member of the American Board of Trial Advocacy (ABOTA) and a recipient of the Florida Justice Association Eagle Centurion Award. The firm’s verified case results are highly indicative of their capacity to handle severe medical evidence, having secured a $13.8 million confidential settlement, a $10.5 million improper surgery outcome, a $10 million verdict regarding improper brain stenting leading to a stroke, a $6.815 million settlement for failure to diagnose Wernicke-Korsakov Syndrome, and $1.45 million for medication errors. By applying this high-level medical malpractice expertise to elder care, the Gunn Law Group effectively holds facilities accountable for medication errors, physical abuse, and clinical neglect.
Stockham Law Group, P.A.
Based in Tampa with a law office located at 109 S.
Stockham Law Group
Located on Edison Avenue, the Stockham Law Group is spearheaded by Donna DeVaney Stockham, an attorney with over two decades of experience and a continuous AV Preeminent rating through Martindale-Hubbell. Stockham’s career trajectory is highly specialized; after graduating law school, she joined Carlton Fields, P.A., where she represented massive pharmaceutical companies in complex Products Liability Group litigation, specifically handling the Fen Phen and Latex Glove mass torts. Seeking to diversify her experience, she transitioned to plaintiff’s work, joining the Merlin Law Group to represent plaintiffs in complex property damage cases across Florida and Texas before founding her own firm in 2013.
This deep background in sophisticated, large-scale insurance litigation perfectly translates into her firm’s secondary focus on nursing home and ALF abuse. Stockham Law Group excels at identifying the subtle “red flags” of abuse—such as frequent infections, unexplained elopements, and cognitive decline—and holding ALFs accountable for accepting residents and payment sources while simultaneously failing to provide adequate healthcare. Stockham serves on the Board of Governors of The Federal Association for Insurance Reform (FAIR) and is recognized as a Florida Super Lawyer, cementing her status as a premier litigator in the Hillsborough region.
Senior Justice Law Firm
With offices positioned strategically throughout Florida, including the Tampa Bay area, Senior Justice Law Firm is entirely unique in its operational structure: the firm narrowly and exclusively focuses on elder abuse and neglect litigation. The firm refuses to handle general auto accidents or standard slip-and-falls; their entire corporate infrastructure, medical expert network, and litigation strategy are hyper-optimized for suing nursing homes and ALFs. Trial Attorney Ryan Dwyer, a Stetson University College of Law graduate who operates heavily within the Palm Beach and Tampa jurisdictions, has established a formidable reputation for prosecuting complex facility negligence cases statewide.
The firm leverages more than half a century of combined courtroom experience to recover tens of millions on behalf of wrongfully injured elderly clients. Their litigation strategy heavily emphasizes meticulous pre-suit investigation. Before ever filing the statutory Chapter 400 notice, the firm analyzes a facility’s historic Medicare health inspection results, federal staffing levels, and quality measure evaluations via the federal Medicare website to establish a provable pattern of historical negligence. They are particularly adept at prosecuting complex pressure ulcer claims, successfully negotiating settlements ranging from $30,000 for early-stage sores to exceeding $1 million for catastrophic Stage 4 ischemic injuries.
The Ruth Law Team
The Ruth Law Team brings over 40 years of personal injury and medical malpractice litigation experience to the arena of elder justice. Led by veteran attorneys such as Steve Ruth, the firm utilizes a massive infrastructure and an extensive geographic footprint to aggressively pursue compensation. They maintain a sprawling network of offices across Florida—including their main office in St. Petersburg, a Tampa office at 511 W Bay Street, and locations in Clearwater, Inverness, Bradenton, Orlando, Sarasota, New Port Richey, and Jacksonville—as well as out-of-state offices in Georgia and Minnesota. Their approach emphasizes highly ethical, unvarnished communication with clients, fundamentally refusing to rely on the generic, algorithmic settlement formulas utilized by insurance companies, and prioritizing long-term outcomes over quick payouts.
Kohn Law, P.A.
Located at 3004 W Cypress St in Tampa, Kohn Law is directed by managing partner Kimberley M. Kohn. Commencing her legal career as an Assistant Public Defender in Tampa, Kohn developed rigorous, battle-tested trial advocacy skills in high-pressure environments. Since 1999, she has focused her private practice entirely on representing victims of nursing home abuse, medical malpractice, and institutional neglect. Kohn is continually recognized by Florida Trend’s Legal Elite, representing fewer than 1.5% of active Florida Bar members. Client reviews consistently highlight the firm’s extreme transparency, prompt communication, and ability to negotiate settlements that exceed initial expectations, particularly in complex medical cases involving hospital-acquired and nursing home-acquired bedsores and severe dehydration.
Conclusions
The crisis of elder abuse and systemic neglect in Tampa and throughout the state of Florida represents an urgent intersection of demographic vulnerability and ruthless corporate healthcare economics. As the elderly population continues to surge across the Gulf Coast, for-profit nursing homes and assisted living facilities frequently compromise patient safety through chronic understaffing, inadequate clinical training, and the prioritization of profit margins. This corporate architecture directly results in devastating, entirely preventable outcomes, including severe malnutrition, fatal unmonitored falls, and catastrophic Stage 4 pressure ulcers.
Florida’s legislative framework, firmly anchored by Chapters 400 and 429, provides robust mechanisms for accountability, empowering residents and their estates to seek both compensatory and punitive damages when their fundamental rights are violated. However, the procedural hurdles—specifically the stringent two-year statute of limitations and the complex 75-day pre-suit notice and informal discovery requirement—demand highly specialized legal navigation to avoid summary dismissal. The recent revival of legislation (HB 6017) permitting the recovery of non-economic pain and suffering damages for adult children and parents in medical negligence wrongful death cases further amplifies the financial stakes, fundamentally expanding the settlement potential of these claims.
The valuation of these lawsuits, particularly concerning ischemic bedsores, is heavily dependent on the clinical severity of the wound and the attorney’s ability to incontrovertibly prove corporate negligence through the subpoenaing of facility payrolls and missing treatment logs. Settlements and verdicts routinely reach into the multi-million dollar range when intentional neglect, sexual abuse, or gross corporate cost-cutting is exposed before a jury. Consequently, the role of specialized Tampa-based elder neglect attorneys—such as those operating at Ford, Dean & Rotundo, Whittel & Melton, Gunn Law Group, Stockham Law Group, Senior Justice Law Firm, The Ruth Law Team, and Kohn Law—is indispensable. By combining aggressive trial advocacy, deep medical pathophysiology knowledge, and the ability to dismantle complex, multi-layered corporate structures, these legal advocates ensure that negligent facilities are held financially accountable, thereby forcing systemic improvements in the standard of care for Florida’s most vulnerable citizens.


